Virtual Health and Health Equity
A perspective on opportunities to improve equity in the design and deployment of virtual health programs

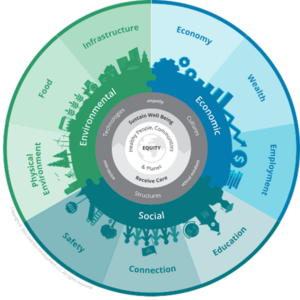
Health equity, the ability to fulfill our human potential in all aspects of health and well-being, is intrinsically tied to our social, economic, and environmental context (see Figure 1) 1. Virtual health (VH) can transform existing care models to improve access, continuity of care, and care management. However, organizations should closely examine how social determinants of health (SDoH) 2 impact their populations and how VH programs – if not implemented intentionally with equity as a guiding principle – may lead to widening the digital divide and increasing health inequities for certain population groups.
As virtual care continues to transform care delivery, organizations should consider key challenges that may compound existing health inequities. Below are three key areas to consider as well as some immediate actions healthcare organizations can take to improve equity in VH programs.
Three key areas to consider:
- Digital literacy and engagement: Digital literacy gaps are high among populations already facing poor health outcomes such as disparate ethnic groups, low-income individuals, and the elderly. Additionally, longstanding challenges with patient engagement related to cultural and language barriers, poor accessibility, and varying levels of trust can be exacerbated in a virtual environment. 34 Only about 50% of Medicaid recipients are digitally literate (e.g., comfortable finding, evaluating, and composing information through digital platforms). 3
- Recommended Actions: Understand the unique barriers to access and engagement among member / patient / user populations and apply human-centered design approach to design VH solutions that enhance customer utilization and engagement. Additionally, actively consider how to implement or operationalize the virtual tools.
- Technology and analytics: Technology and analytics have the potential to exacerbate discrimination if not designed with equity in mind. Bias embedded within AI for speech and facial recognition and choice of data proxies for healthcare prediction algorithms can lead to inaccurate predictions resulting in suboptimal outcomes, access or engagement among certain populations. 67A study of a commercial health system prediction algorithm was shown to underestimate the number of Black patients in need of greater care by half. Removal of bias resulted in this estimation to increase from 17.7% to 46.5%. 7
- Recommended Actions: Audit capabilities involved in developing and deploying VH to help ensure equity is actively considered, address immediate biases identified by redesigning the relevant part of the data cycle, and design an organizational ethical framework using commonly agreed upon standards of fairness and equity.
- Equitable infrastructure: Lack of access to adequate broadband, necessary equipment, and appropriate physical environment creates barriers to VH utilization, especially impacting rural populations, low-income populations, and certain racial groups. 35 Studies have found that 26% of Medicare beneficiaries, including 37% of Black Medicare beneficiaries, lack access to a smartphone with a data plan or an internet-connected computer.5
- Recommended Actions: Determine what health equity policy priorities are most closely aligned with organization’s VH strategy and ambition and develop a policy agenda that promotes equitable delivery of VH solutions, work with partners to set up connectivity zones and provide needed resources to customers.
More broadly, we recommend that organizations intentionally embed health equity into their VH programs by considering critical components of their programs through an equity lens:
- Strategy & Governance: Is health equity explicitly called out as a core principle in the VH program vision?
- Operations & Workflow Integration: How is the identification of and support with unmet social needs / SDoH barriers integrated into VH workflows and program planning?
- Care Model Design: How are person-centered care models designed to consider people across demographic segments?
- Business Model: What is the organization doing to advance public policy that enables reimbursement of services critical for equitable access to VH?
- Customer Experience: How can the organization offer a differentiated experience by addressing SDoH and delivering with a diverse workforce that meet the needs / preferences of customers?
- Workforce Readiness: How can clinical and non-clinical workforce be trained to better mitigate engagement barriers to VH faced by different customer segments?
- Technology Infrastructure & Interoperability: How can the organization integrate health equity considerations in design of solutions and vendor selection?
- Cognitive & Analytics: How might bias in analytics impact outcomes and engagement with VH solutions?
Placing an emphasis on equity across all capabilities of a VH program can lead to virtual solutions that are more accessible for all customers, lead to better outcomes for virtual and digital care modalities, and provide a better experience, thereby promoting better health outcomes overall.
For more information, check out Deloitte’s Health Equity Institute page.
This publication contains general information only and Deloitte is not, by means of this publication, rendering accounting, business, financial, investment, legal, tax, or other professional advice or services. This publication is not a substitute for such professional advice or services, nor should it be used as a basis for any decision or action that may affect your business. Before making any decision or taking any action that may affect your business, you should consult a qualified professional advisor.
Deloitte shall not be responsible for any loss sustained by any person who relies on this publication.
About Deloitte
Deloitte refers to one or more of Deloitte Touche Tohmatsu Limited, a UK private company limited by guarantee (“DTTL”), its network of member firms, and their related entities. DTTL and each of its member firms are legally separate and independent entities. DTTL (also referred to as “Deloitte Global”) does not provide services to clients. In the United States, Deloitte refers to one or more of the US member firms of DTTL, their related entities that operate using the “Deloitte” name in the United States and their respective affiliates. Certain services may not be available to attest clients under the rules and regulations of public accounting. Please see www.deloitte.com/about to learn more about our global network of member firms.
Copyright © 2021 Deloitte Development LLC. All rights reserved.
Blog Authors
- Tiffany Lin, Sima Muller, Heather Nelson
- PPMD Sponsor: Bill Fera
Citations:
1. No one should be surprised that low-income populations are being hit harder by COVID-19: How do we achieve health equity? Deloitte, October 15, 2020
2. What We Need To Be Healthy—And How To Talk About It, Health Affairs, May 3, 2021
3.Why achieving health equity is so hard in the telehealth age, AMA, October 21, 2020
4.Web Content Accessibility Guidelines (WCAG) 2.1, W3C, June 5, 2018
5. Assessment of Disparities in Digital Access Among Medicare Beneficiaries and Implications for Telemedicine, JAMA, August 3, 2020
6. HUD v. Facebook, HUD, March 29, 2019
Dissecting racial bias in an algorithm used to manage the health of populations, AAAS, October 25, 2019


